Shingles Herpes Zoster
Shingles is a painful rash caused by an infection of a nerve underneath the skin with the varicella-zoster virus.
What is shingles?
What is shingles?
Shingles is a painful, blistery rash in one specific area of your body. Most of us get chickenpox in our lives, usually when we are children. Shingles is a reactivation of that chickenpox virus but only in one nerve root. So instead of getting spots all over your body, as you do when you have chickenpox, you get them just in one area of your body.
It is almost always just on one side of your body, although it may go right around from front to back, following the skin the nerve affects. The affected skin hurts, and it may start to hurt before the rash appears, and may keep hurting for some time after the rash has gone. You may feel generally off-colour and not yourself.
What are the symptoms of shingles?
Shingles symptoms occur in the area of skin that is supplied by the affected nerve fibres. The usual symptoms are pain and a rash. Occasionally, two or three nerves next to each other are affected.
Very rarely, shingles can cause more widespread infection, or can affect both sides of the body, but this is usually only in people with a weakened immune system.
The most commonly involved nerves are those supplying the skin on the chest or tummy (abdomen). The upper face (including an eye) is also a common site.
Pain
The shingles pain is a localised band of pain. It can be anywhere on your body, depending on which nerve is affected. The pain can range from mild to severe. You may have a constant dull, burning, or gnawing pain. In addition, or instead, you may have sharp and stabbing pains that come and go. The affected area of skin is usually tender.
Rash
The shingles rash typically appears 2-3 days after the pain begins. Red blotches appear that quickly develop into itchy fluid-filled blisters. The rash looks like chickenpox but only appears on the band of skin supplied by the affected nerve. New blisters may appear for up to a week. The soft tissues under and around the rash may become swollen for a while due to inflammation caused by the virus. The blisters then dry up, form scabs and gradually fade away. Slight scarring may occur where the blisters have been. The picture shows a scabbing rash (a few days old) of a fairly bad bout of shingles. In this person, it has affected a nerve and the skin that the nerve supplies, on the left side of the abdomen.
Is shingles contagious?
You cannot get shingles from someone who has shingles. You can catch chickenpox from someone with shingles if you have not had chickenpox before. But most adults and older children have already had chickenpox and so are immune from catching chickenpox again.
The shingles rash is contagious (for someone else to catch chickenpox) until all the blisters (vesicles) have scabbed and are dry. If the blisters are covered with a dressing, it is unlikely that the virus will pass on to others. This is because the virus is passed on by direct contact with the blisters.
Can I go to work with shingles?
If you have a job, you can return to work once the blisters have dried up, or earlier if you keep the rash covered and feel well enough. Similarly children with shingles can go to school if the rash is covered by clothes and the children do not feel unwell.
Which groups to avoid if you have shingles
Pregnant women who have not had chickenpox should avoid people with shingles. See the separate leaflet called Chickenpox Contact in Pregnancy for more details. Also, if you have a poor immune system (immunosuppression), you should avoid people with shingles. (See below for a list of people who have a poor immune system.) These general rules are to be on the safe side, as it is direct contact with the rash that usually passes on the virus.
Can other people catch shingles?
This one is confusing! You can catch chickenpox from other people, but you can't catch shingles from other people. You only get shingles from a reactivation of your own chickenpox infection in the past.
So if you have shingles, and you come into contact with somebody else, they cannot 'catch' your shingles. But if they have never had chickenpox, it is possible that they could catch chickenpox from you. (And if you had chickenpox, and came into contact with somebody else who had never had chickenpox, they could catch chickenpox. But they couldn't 'catch' shingles from your chickenpox.)
To put it another way, no, you don't 'catch' shingles. It comes from a virus hiding out in your own body, not from someone else. But if you have shingles, you may be infectious, as it is possible for people to catch chickenpox from you.
Only people who have never had chickenpox are likely to be at risk of catching chickenpox from your shingles. People who have had chickenpox should be immune from catching it again. If the rash is in a covered area of skin, the risk of anyone with whom you are not in close contact catching chickenpox is very low.
What does shingles look like?
Shingles appears as red blotches, usually on your chest or stomach. These rashes develop into blisters filled with fluid and will only appear on one side of your body. If they appear on both sides of your body, it's not likely to be shingles causing the problem.
Shingles Day 2
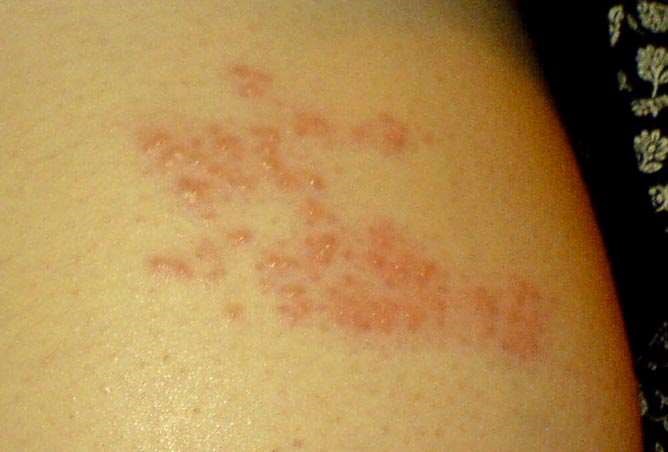
Shingles Day 6
Images above by Mariegriffiths via Wikimedia Commons
How long does shingles last?
An episode of shingles usually lasts 2-4 weeks. In some cases there is a rash but no pain. Rarely, there is no rash but just a band of pain.
You may also feel you have a high temperature (feel feverish) and feel unwell for a few days.
Book a pharmacy appointment today
Did you know your local pharmacist can provide treatment for shingles? Book a consultation today
How common is shingles?
Shingles is an infection of a nerve and the area of skin supplied by the nerve. It is caused by a virus called the varicella-zoster virus. It is the same virus that causes chickenpox. Anyone who has had chickenpox in the past may develop shingles. Shingles is sometimes called herpes zoster. (Note: this is very different to genital herpes which is caused by a different virus called herpes simplex.)
About 1 in 4 people have shingles at some time in their lives. It can occur at any age but it is most common in older adults (over the age of 50 years). After the age of 50, it becomes increasingly more common as you get older. It is uncommon to have shingles more than once but some people do have it more than once.
Causes of shingles
Most people have chickenpox at some stage (usually as a child). The virus does not completely go after you have chickenpox. Some virus particles remain inactive in the nerve roots next to your spinal cord. They do no harm there and cause no symptoms. For reasons that are not clear, the virus may begin to multiply again (reactivate). This is often years later. The reactivated virus travels along the nerve to the skin to cause shingles.
In most cases, an episode of shingles occurs for no apparent reason. Sometimes a period of stress or illness seems to trigger it. A slight ageing of the immune system may increase the risk of developing shingles and account for it being more common in older people. (The immune system keeps the virus inactive and prevents it from multiplying. A slight weakening of the immune system in older people may account for the virus reactivating and multiplying to cause shingles.)
The risk of getting shingles increases in people with a poor immune system (immunosuppression). For example, shingles commonly occurs in younger people who have HIV/AIDS or whose immune system is suppressed with treatment such as steroids or chemotherapy.
How to treat shingles
Two main aims of treating shingles are:
- To ease any pain and discomfort during the episode of shingles.
- To prevent shingles, as much as possible, complications from developing.
General measures to alleviate shingles symptoms
Loose-fitting cotton clothes are best to reduce irritating the affected area of skin. Pain may be eased by cooling the affected area with ice cubes (wrapped in a plastic bag), wet dressings, or a cool bath. A non-adherent dressing that covers the rash when it is blistered and raw may help to reduce pain caused by contact with clothing. Simple creams (emollients) may be helpful if the rash is itchy. Calamine lotion can help to cool the skin and reduce mild itchiness.
Painkillers for shingles
Painkillers - for example, paracetamol, or paracetamol combined with codeine (such as co-codamol), or anti-inflammatory painkillers (such as ibuprofen) - may give some relief for shingles. Strong painkillers (such as oxycodone and tramadol) may be needed in some cases.
Some painkillers are particularly useful for nerve pain. If the pain during an episode of shingles is severe, or if you develop postherpetic neuralgia (PHN), you may be advised to take:
- An antidepressant medicine in the tricyclic group. An antidepressant is not used here to treat depression. Tricyclic antidepressants, such as amitriptyline, imipramine and nortriptyline, ease nerve pain (neuralgia) separate to their action on depression; or
- An anticonvulsant medicine such as gabapentin or pregabalin. They also ease neuralgic pain separate to their action to control convulsions.
If an antidepressant or anticonvulsant is advised, you should take it regularly as prescribed. It may take up to two or more weeks for it to become fully effective to ease pain. In addition to easing pain during an episode of shingles, they may also help to prevent PHN. See the separate leaflet called Postherpetic Neuralgia for more information.
Antiviral medicines for shingles
Antiviral medicines used to treat shingles include aciclovir, famciclovir and valaciclovir. An antiviral medicine is not a cure for shingles, it does not kill the virus but works by stopping the virus from multiplying. So, it may limit the severity of symptoms of the shingles episode.
An antiviral medicine is most useful when started in the early stages of shingles (within 72 hours of the rash appearing). However, in some cases your doctor may still advise you have an antiviral medicine even if the rash is more than 72 hours old - particularly in elderly people with severe shingles, or if shingles affects an eye.
Antiviral medicines are not advised routinely for everybody with shingles. As a general rule, the following groups of people who develop shingles will normally be advised to take an antiviral medicine:
- If you are over the age of 50. The older you are, the more risk there is of severe shingles or complications developing and the more likely you are to benefit from treatment.
- If you are of any age and have any of the following:
- Shingles that affects the eye or ear.
- A poorly functioning immune system (immunosuppression - see later for who is included).
- Shingles that affects any parts of the body apart from the trunk (that is, shingles affecting an arm, leg, neck, or genital area).
- Moderate or severe pain.
- Moderate or severe rash.
If prescribed, a course of an antiviral medicine normally lasts seven days.
Steroid medication for shingles
Steroids help to reduce swelling (inflammation). A short course of steroid tablets (prednisolone) may be considered in addition to antiviral medication. This may help to reduce pain and speed healing of the rash. However, the use of steroids in shingles is controversial. Your doctor will advise you. Steroids do not prevent PHN.
Are there any tests for shingles?
Tests are not usually done for shingles. The rash can be recognised by its typical pattern and symptoms.
Should I see a doctor for shingles?
It is usually worth seeing a doctor to be certain about the diagnosis and to see if you need treatment or not. Ideally you should see a doctor as soon as possible after the rash appears.
The rash of shingles can be very painful. So even if the doctor doesn't think you need an anti-shingles medicine, they may be able to give you stronger painkillers than those you can buy over the counter from the chemist.
Shingles and pregnancy
There's no danger to you or your baby if you catch shingles while pregnant. However, you may need antiviral treatment so you should be referred to a specialist.
What if I have shingles and a poor immune system?
If you have a poor immune system (immunosuppression) and develop shingles then see your doctor straightaway. You will normally be given antiviral medication whatever your age and will be monitored for complications. People with a poor immune system include:
- People taking high-dose steroids. (This means adults taking 40 mg prednisolone (steroid tablets) per day for more than one week in the previous three months. Or, children who have taken steroids within the previous three months, equivalent to prednisolone 2 mg/kg per day for at least one week, or 1 mg/kg per day for one month.)
- People on lower doses of steroids in combination with other immunosuppressant medicines.
- People taking anti-arthritis medications which can affect the bone marrow.
- People being treated with chemotherapy or generalised radiotherapy, or who have had these treatments within the previous six months.
- People who have had an organ transplant and are on immunosuppressive treatment.
- People who have had a bone marrow transplant and who are still immunosuppressed.
- People with an impaired immune system.
- People who are immunosuppressed with HIV infection.
What complications are there from shingles?
Most people who get shingles do not have any complications. Those that sometimes occur include the following.
Postherpetic neuralgia (PHN)
This is the most common complication of shingles. It is where the nerve pain (neuralgia) of shingles persists after the rash has gone. See the separate leaflet called Postherpetic Neuralgia for more details.
Skin infection
Sometimes the rash becomes infected with germs (bacteria). The surrounding skin then becomes red and tender. If this occurs you may need a course of medicines called antibiotics.
Eye problems
Shingles of the eye can cause inflammation of the front of the eye. In severe cases it can lead to inflammation of the whole of the eye which may causevision loss.
Weakness
Sometimes the nerve affected is a motor nerve (ones which control muscles) and not a usual sensory nerve (ones for touch). This may result in a weakness (palsy) of the muscles that are supplied by the nerve.
Various other rare complications
Examples are infection of the brain by the varicella-zoster virus, or spread of the virus throughout the body. These are very serious but rare. People with a poor immune system (immunosuppression) who develop shingles have a higher than normal risk of developing rare or serious complications. (For example, people with HIV/AIDS, people on chemotherapy, etc.)
Is there a shingles vaccination?
In the UK there is a shingles vaccine immunisation programme for people aged 70 years to protect against herpes zoster. There is also a catch-up programme which offers the vaccine to anyone aged between 70 and 79 years who has previously missed out on immunisation. The vaccine is licensed for people aged over 50 years, and if you are not eligible for the vaccine on the NHS, your pharmacist may be able to provide the vaccine as a private (paid for) service.
The chickenpox vaccine is not routinely given to children in the UK but is offered to people who are in close contact with someone who is particularly vulnerable to chickenpox or its complications - eg, people with a weakened immune system.
Further reading and references
Immunisation against infectious disease - the Green Book (latest edition); UK Health Security Agency.
Shingles; NICE CKS, September 2019 (UK access only)
Who is eligible for the shingles vaccine beyond 2016; Public Health England